On Wednesday 9th June, after a COVID test and self isolation, I was a planned admission to the Neuromuscular Complex Care unit at the National Hospital in Queen Square for a respiratory assessment. Apart from inadvertently driving into a vehicle free zone in Tottenham Court Road on the way, we had an uneventful journey (I’m still waiting for the Penalty Charge Notice to arrive!)
With MND the muscles that control breathing become compromised. This causes shallow breathing, which leads to a decreased oxygen level in the blood and a build up of carbon dioxide in the lungs (particularly at night). During my two day stay in hospital I learnt that the latter problem is actually the more serious. The answer is to use a ventilator that gently pushes fresh air into the lungs in a rhythmic breathing pattern. If done overnight the chances are that you’ll wake up feeling much more refreshed.

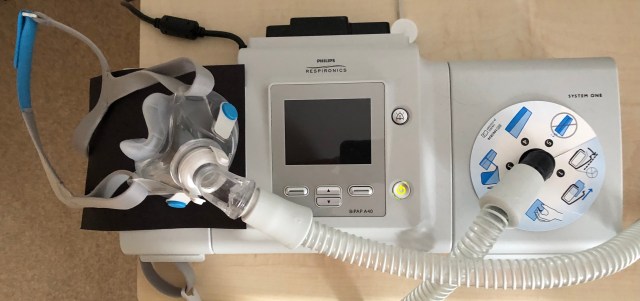
After a series of blood tests, and an arterial oxygenation test, I was introduced to my Philips A40 BiPap machine and face mask. The mask is incredibly uncomfortable to start with and you really wonder how on earth you’ll be able to sleep! But it has to be tight to prevent excessive leakage. My first session (in the afternoon) was of about 30 minutes duration – long enough to begin to get used to the ventilator and to learn how to breathe at the same rate as the machine.
It’s a very clever device and, via a two way inbuilt modem, the hospital team can monitor my use of the machine and make adjustments to the ventilator settings.
The first night sleeping with the ventilator was very difficult. In addition to wearing the mask, I had a blood oxygen sensor attached to my right ear (and earphones in my ears to give me something soothing to listen to). Once back home things did become easier and, alongside taking medication and flushing my PEG, putting on the mask and setting the machine were added to the bedtime routine.
For about two weeks I found I could manage to sleep reasonably well using the face mask for about four hours most nights, and then would abandon it for the second half of the night. Then I encountered a problem, which is still being investigated – excessive amounts of saliva. Unfortunately, this has stopped me using the ventilator for the time being. Many people living MND find they have more saliva and mucus congestion than normal, and it tends to be quite thick and tenacious. When I’m lying down (even in an elevated position) it’s very hard to swallow and to clear. So, with mouth slightly open because of weakened muscles, saliva finds its way into the mask giving the sensation of drowning.
I’m trying various medications which are supposed to have the effect of reducing the problem of saliva secretions. Hopefully this will be sorted in July, allowing me to resume nightly use of the ventilator.
Other news in brief
In other news this month, I’ve noticed that my legs are much weaker now – to the point where it’s getting very hard to stand up from sitting (this adds many complications to life) and I no longer trust my hands to carry a drink or a plate of food. So it’s now two hands for every job – my left hand supporting my right. So a straight beer glass has been replaced by a light plastic one one with a handle, and the time is coming when I will need an arm support machine to help me raise a fork to my mouth. As I’ve written before, it important for me to try to stay one step ahead of looming problems. You can’t beat MND, but you can prepare, and this in itself gives some small degree of satisfaction.
Finally, we had a lovely time in Dorset over two days with my sister Jill and brother in law David. Kimmeridge Bay was stunning at low tide on a mid summer Wednesday morning, making life a lot more bearable.

